To those who work hard to de-stigmatize sex education, to normalize sexual behavior, to promote pleasure, make lessons inclusive, and have the confidence to do all of that while injecting in some humor – you are my heroes. If you are one of those educators, or striving to become one, I present to you, Ina Park – physician, medical consultant on STI’s to the CDC, past owner of a giant condom outfit, and author of the awesome new book “Strange Bedfellows. Adventures in the Science, History, and Surprising Secrets of STD’s“. Look out for the chance to win a copy of Ina’s book at the bottom of the page.

How can we #stopSTIgma? Changing the conversation around sexually transmitted infections (STIs)
Before the COVID-19 pandemic, the United States was experiencing an epidemic of sexually transmitted infections (STIs), with 2019 being the highest year on record for reported STIs, according to the Centers for Disease Control and Prevention. For many of us who are educators today, our own introduction to STIs consisted of slide shows of the worst-case-scenarios for every infection/disease, a veritable parade of unhappy genitals. This was effective at inducing fear and perpetuating the stigma that surrounded STIs, making us feel that if we were to be diagnosed, this could lead to rejection and judgement from peers and partners.
As evidenced by our skyrocketing STI rates in the US, the old ways of teaching about STIs have not served us well. So what can we do to rewrite the narrative around STIs for today’s current generation of learners?
Language Matters: VD vs STD vs STI
In the US, the term “venereal disease” or VD was in vogue before the 1970s. It was a term that implied that “venery” or immoral behavior was involved in disease transmission. The 1970s ushered in the era of “sexually transmitted diseases (STDs),” a term felt to be a less stigmatizing than VD. We were happy with “STDs” for a while. But in the 1990s, there was growing recognition that many sexually transmitted bugs were silent infections that resolved spontaneously, meaning they didn’t cause disease (e.g. human papillomavirus-HPV). Thus, the term “sexually transmitted infection” or “STI” came onto the scene. Among researchers/academics, both terms are used because many of us study both the infections and the diseases they cause. For those of us who are working with students/learners, I recommend using the term “STI.” It’s scientifically more accurate, as most of these infections will hopefully not result in disease, and may be less stigmatizing than being labeled as having an “STD.”
Debunk common myths
Contrary to popular belief, catching an STI often isn’t related to how many people one has sex with, but rather what sexual networks they happen to be a part of. Sexual networks describe the sexual connections between people in a given span of time: you are having sex with the person in front of you, plus everyone they’ve slept with in a certain span of time (the time span varies for different STIs). For a bacterial STI such as gonorrhea/chlamydia, even having one partner can mean very different levels of risk depending on how many people that person has had sex with over the past two months.
Check out the example below with Caroline and Alice. Each would say “I only have one sex partner.” But while Alice’s partner has only been connected with her in the past two months, Caroline’s partner was sexually connected to 14 other partners in addition to Caroline. (Educators, if you’d like to use this diagram, please feel free)
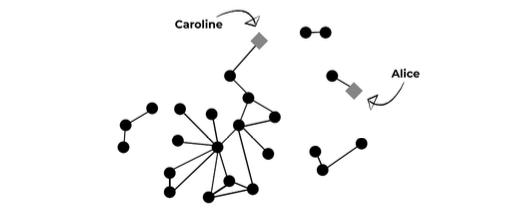
The number of sexual connections is only part of the story. In a population with low rates of disease, it’s possible for someone to have many partners and never catch an STI. On the other hand, in networks with higher disease rates, even having two partners may result in multiple repeated STIs. The prevalence of an STI (how common the infection is) in a sexual network is affected by the characteristics of its members, including: age, sexual orientation, geography, poverty/access to healthcare, incarceration of males in the community, and other social factors that go beyond the simple act of sex between two people.
If someone is catching STIs repeatedly, it’s a sign that they’re having sex in a high-prevalence network. Using barriers such as condoms is crucial to avoid multiple repeated infections that can lead to complications from STIs, particularly for people who were assigned female at birth.
Normalize STIs
In January 2021, the CDC estimated that one in five Americans (68 million people) have an STI, with half of all new STIs occurring in young people between the ages of 15-24. Viral STIs such as human papillomavirus are so common, almost every sexually active person will be exposed at some point during their lives. Normalizing STIs is key when teaching about them: “Every person in this room who has sex is going to catch an STI from someone, someday. You won’t always realize when it happens, but it does. Catching an STI simply means you are a sexual human being. That’s it.” My advice to my patients, other than using barrier methods such as condoms, is trying to have healthy relationships. While mutual, consensual, pleasurable relationships don’t shield anyone from catching an STI, they make it less likely that someone will feel regret if they happen to be diagnosed.
Will normalizing STIs help us defeat STI-related stigma? I don’t know, but we must start somewhere. We’ve managed to defeat stigma surrounding previously taboo subjects such as cancer, creating discourse and shifting public sentiment towards support rather than shame. We need a similar sea change around STIs to have any hope of curbing the current epidemic.
Website: http://inapark.net
Twitter: @InaParkMD
LinkedIn: https://www.linkedin.com/in/ina-park-45044766/
I highly recommend that you check out Ina’s new book, and if you know a sexuality educator who ISN’T working hard to de-stigmatize sex education, normalizing sexual behavior, promoting pleasure, making lessons inclusive, and doesn’t have the confidence to do all of that while injecting in some humor….BUY THEM A COPY.

“Strange Bedfellows. Adventures in the Science, History, and Surprising Secrets of STD’s” discusses the lingering stigma of genital herpes, the stunning success of HPV vaccination, the hazards of pubic hair removal, and the dangers of douching. You’ll learn of epidemic increases in congenital syphilis and the threat of antibiotic-resistant gonorrhea. And don’t forget the promise of prophylaxis, for both HIV and STIs. Check out the New York Times review of Strange Bedfellows and share your thoughts with our #HealthEd community.

Pingback: Love Safe, Get Tested: A Valentine’s Day Reminder – #slowchathealth
Pingback: Lyme Disease – #slowchathealth
Pingback: 12 Books Under $12 – #slowchathealth